Lorem ipsum dolor sit amet consectetur adipiscing elitsed do eiusmod tempor incididunt utlabore et dolore magna aliqua. Utenim ad minim veniam quis nostrud exercitation ullamco laboris.

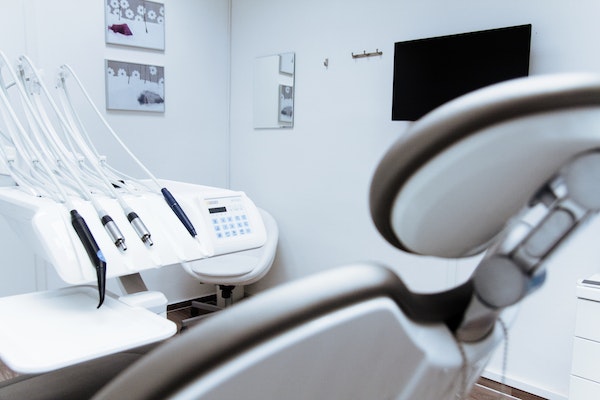
ATS HEALTHCARE
Maximize Your Practice's
Efficiency with AI - Driven
Solutions

ATS HEALTHCARE
Your One-Stop Shop for
Comprehensive Medical Billing
and Transcription Solutions

ATS HEALTHCARE
Medical Excellence:
A Legacy of Trust Built Over
15+ Years and 60+ Years of
Combined Industrial Expertise!

Our Values and Goals
ABOUT US
We are guided by our core values of integrity, excellence, innovation, and collaboration. Our primary goal is to deliver exceptional value to our clients by helping them maximize their revenue and improve patient care through our medical billing and transcription solutions. We are committed to driving efficiency and streamlining operations, utilizing the latest technology and processes to help our clients save time and reduce costs. We strive to foster growth and success for our clients by providing expert guidance and support every step of the way, and building strong, long-term relationships based on personalized service and support.
Core Technology services
OUR SERVICES
Request a free
consultation with us
CONTACT US NOW
Schedule a free consultation with us and discover how our customized solutions can optimize your practice's revenue and efficiency.
Areas of Expertise
RURAL HEALTH CLINICS | PSYCHIATRY | DERMATOLOGY |
What our clients thinks
TESTIMONIALS FEEDBACK
Latest News & Blogs
Read Blog


 Albert Patterson
Albert Patterson